Full Mouth Dental Implants: Treatment Analysis, Clinical Scenarios & Outcomes
A clinical analysis of full mouth dental implants: when they are genuinely indicated, when they are not, treatment pathways, ethical decision-making, and what separates durable outcomes from early failures.

Full mouth dental implants are often discussed as a definitive solution, yet in clinical reality they represent a narrow, carefully defined indication rather than a universal answer. This page was written for patients who want clarity, not reassurance — and for those willing to understand whether implants are truly necessary, or simply appealing.
What follows is not designed to convince, but to filter, explain, and protect long-term outcomes through clinical reasoning rather than visual promise.
Full Mouth Implants Are Structural Reconstruction — Not a Smile Makeover
One of the most damaging misconceptions in modern dentistry is the idea that implants are an enhanced version of cosmetic dentistry. They are not.
Veneers, crowns, aligners, and minimally invasive smile makeovers are preservative treatments. Their goal is to protect and optimise what already exists. Implants, by contrast, replace what has been lost — teeth, roots, and often the supporting architecture that once maintained facial balance.
When full mouth implants are proposed, it usually means that at least one of the following has already occurred: - Long-term tooth loss with progressive bone resorption - Repeated restorative failures - Advanced periodontal compromise - Occlusal collapse altering chewing mechanics and facial proportions
In other words, implants do not enhance a smile — they rebuild a system. This distinction matters because outcomes depend less on visual inspiration and more on biological readiness: bone density, load distribution, healing capacity, and long-term functional planning.
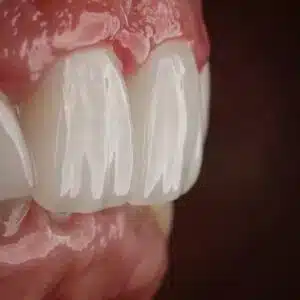
The Biological Threshold: When Implants Become the Rational Option
Clinicians do not ask, 'How can we place implants?' They ask, 'At what point do natural structures stop serving the patient predictably?'
Three clinical markers signal this transition:
**Tooth viability** — Teeth that require repeated root canal treatments, crowns, or repairs may appear salvageable, but structurally they are already compromised. When cumulative interventions weaken long-term prognosis, replacement becomes safer than preservation.
**Bone integrity** — Bone loss does not simply affect implant placement; it alters facial support. Once bone resorption accelerates, delayed intervention often leads to more complex reconstruction requiring more grafting and more invasive procedures.
**Functional load and occlusion** — A stable bite distributes forces evenly. When teeth are missing or misaligned, load concentrates in unhealthy patterns, accelerating failure. Implants restore not just teeth, but force balance.
Patients who reach this threshold often describe subtle but persistent issues: difficulty chewing, jaw fatigue, shifting teeth, facial shortening, or a sense that their bite no longer feels 'right.' These are not cosmetic complaints — they are functional warnings.

When Implants Are Chosen for the Wrong Reasons
A significant portion of dissatisfaction after full mouth implant treatment does not stem from surgical failure, but from incorrect indication. The most problematic cases are rarely those with advanced collapse — they are cases where implants were chosen too early, too aggressively, or for reasons unrelated to structural necessity.
The most common non-clinical drivers include: - Fatigue from repeated cosmetic maintenance - Frustration after multiple minor restorations - Aesthetic comparison with public figures - Marketing narratives that frame implants as a permanent upgrade
None of these are biological indications. Implants respond to loss — not to impatience.

Preservation vs Replacement: The Ethical Foundation
From a clinical standpoint, dentistry operates on a simple hierarchy: preserve first, replace last. This principle exists because no artificial structure, regardless of sophistication, replicates the sensory feedback, adaptive capacity, and biological integration of natural teeth.
Experienced clinicians therefore ask: 'What can we still save — and for how long?' If preservation can offer predictable function for years, replacement is postponed. This is not conservatism for its own sake; it is risk management.
Replacement introduces new variables: implant-bone interface behaviour, long-term load tolerance, peri-implant tissue stability, and maintenance dependency. Once implants are placed, the patient enters a lifelong maintenance pathway. This commitment should never be framed as convenience.
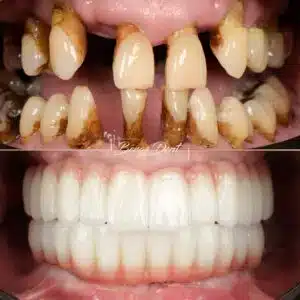
Treatment Pathways: Sequences, Not Packages
Clinically sound treatment planning does not begin with how many implants will be placed. It begins with determining which pathway best aligns with the patient's current condition and future needs.
**Preservation-first pathway** — Applies to patients whose natural teeth, while compromised, remain salvageable with predictable outcomes. The priority is to extend natural dentition while stabilising function. Implants remain a future option but are not the immediate solution.
**Transitional rehabilitation pathway** — For patients in a clinical middle ground: certain teeth may be beyond recovery while others remain viable. Staged extractions, selective implant placement, and gradual occlusal correction. Controlled transition rather than abrupt replacement.
**Full structural rehabilitation pathway** — Full mouth implants become central only when structural collapse is established: extensive tooth loss, advanced bone resorption, unstable occlusion, compromised facial support. Planning emphasises force distribution, prosthetic design, and long-term maintenance strategies.
Biological systems respond over time. Sequenced pathways allow clinicians to reassess bone response, adjust implant positioning, and refine prosthetic design. Precision over time consistently produces better outcomes than rapid completion.
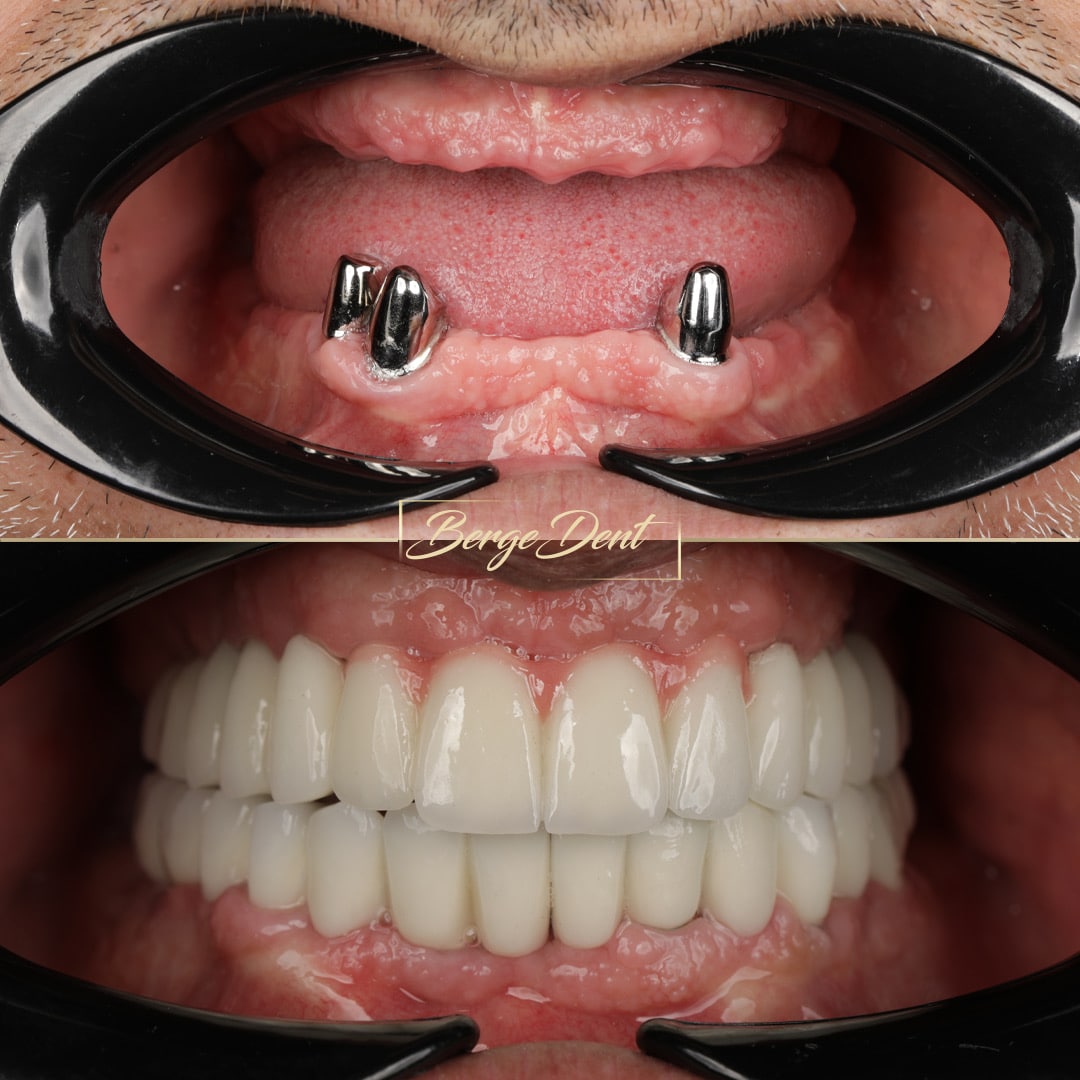
From Celebrity Smiles to Clinical Reality
Celebrity smiles are photographed outcomes, not clinical starting points. What remains invisible are the years of preservation that often precede those results: early orthodontic alignment, conservative restorations, periodontal maintenance, and timely intervention long before structural decline.
In most high-profile cases, implants are avoided for as long as possible. The priority is to protect natural roots and bone, because once they are lost, reconstruction becomes inevitable.
In high-profile dentistry, treatment planning emphasises reversibility and preservation. Implants introduce permanence — not just in structure, but in maintenance obligations and biomechanical commitment. This reframes the decision entirely: implants are not the gold standard of cosmetic dentistry. They are the corrective tool of last resort when preservation no longer serves the patient.
The most productive question is not 'Which smile do I want?' but 'Which clinical category does my dental condition fall into?' — preservation candidate, transitional candidate, or reconstruction candidate. Only the third profile belongs on a full mouth implant pathway.

What Separates Durable Outcomes from Early Failures
Throughout this analysis, one pattern repeats: successful outcomes are not driven by implant counts, brand names, or speed promises. They are driven by alignment — between anatomy, force patterns, prosthetic design, and long-term maintainability.
Patients who arrive at full-arch rehabilitation often share different histories, but face similar decision pressures: instability, repeated failure, declining confidence, or the sense that incremental repair no longer makes sense.
What distinguishes durable solutions is not the absence of future events, but the presence of a system designed to absorb them. When implants are distributed appropriately, when occlusion is controlled, and when maintenance is anticipated rather than denied, risk becomes manageable.
From the patient perspective, the most meaningful outcome is often not a visible transformation, but a subtle one: eating without hesitation, speaking without awareness, and no longer planning daily life around dental limitations.
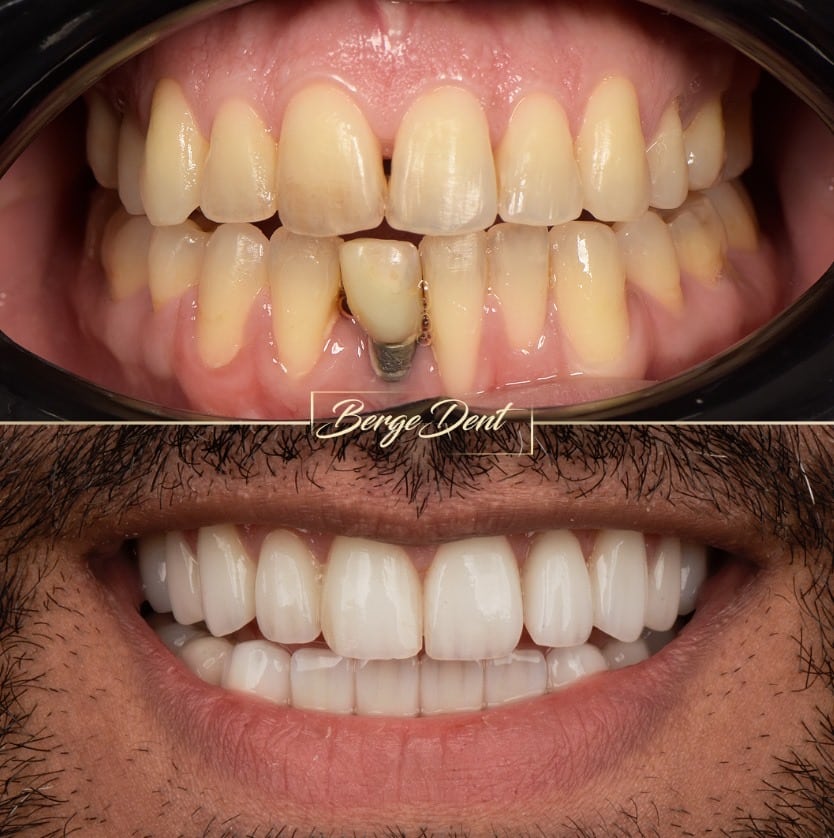
Frequently asked questions
Are full mouth dental implants appropriate for aesthetic improvement alone?
No. Full mouth implants are indicated for structural reconstruction, not cosmetic refinement. If your natural teeth are structurally sound and functional, conservative aesthetic treatments are clinically preferable. Implants should not be used to replace viable teeth for cosmetic reasons.
What is the difference between All-on-4 and All-on-6?
All-on-4 uses four implants to support a full arch, typically with two angulated posterior implants to maximise available bone. All-on-6 uses six implants for greater force distribution. The choice depends on bone volume, force patterns, and clinical judgment — not aesthetic preference.
What happens if implants are placed prematurely?
Premature implant placement can lead to unnecessary extraction of viable teeth, complex future revisions, higher long-term maintenance burden, and dissatisfaction rooted in misaligned expectations. This is why ethical implant planning requires indication criteria, not patient enthusiasm alone.
How do clinicians decide between extraction and preservation?
The decision hinges on long-term prognosis. Teeth with acceptable root integrity, manageable periodontal status, and predictable restoration options are preserved where possible. Teeth with compromised prognosis after cumulative treatment are candidates for replacement.
What should I bring to a full mouth implant consultation?
Bring any existing imaging (panoramic X-ray, CBCT if available), a record of your dental history including past treatments and failures, a list of medications, and specific questions about your bone anatomy and force patterns. NexWell can coordinate a pre-consultation digital review before you travel.
Free Guide: The Complete Medical Tourism Handbook
Cost comparisons, clinic evaluation checklist, packing list & recovery tips — everything you need to plan your treatment in Turkey.
Related reading
dental-treatments
Do I Need Full Mouth Dental Implants? Candidacy Checklist
Learn how dentists evaluate whether full mouth dental implants are appropriate for you — clinical signals, common candidacy profiles, reasons to delay, and questions to ask before deciding.
dental-treatments
Full Mouth Dental Implant Risks and Complications: A Realistic Overview
A clear, clinical overview of full-arch implant risks — biologic, mechanical, and force-related. Understanding complications in advance is what makes long-term outcomes manageable.
dental-treatments
Life After Full Mouth Dental Implants: What It Actually Feels Like
What daily life is really like after full mouth dental implants — eating freely, adapting speech, reduced self-consciousness, and how the experience shifts quietly over months and years.
dental
Full Mouth Dental Implants in Turkey
Restore both upper and lower arches with premium implant systems. All-on-4, All-on-6, or individual implants — your Istanbul implantologist designs the optimal approach for your anatomy and goals.
dental-implant-guides
All-on-4 vs All-on-6 Dental Implants: Which Full-Arch Solution Is Right for You?
A clinical comparison of All-on-4 and All-on-6 full-arch implant systems — load distribution, bone requirements, cost differences, and which option suits your jaw anatomy.
dental-treatments
Dental Implants Turkey Cost 2026: Single, All-on-4 & Full Mouth Guide
A practical cost breakdown for single implants, All-on-4, All-on-6 and full mouth implant cases in Turkey.
Why this page is publishable
Experience signals
- • Developed with input from specialist implantologists at NexWell partner clinics
- • Reflects clinical decision-making frameworks used across full-arch assessment consultations
Trust signals
- • NexWell partner clinics apply the same indication discipline described in this guide
- • This content is designed to filter, not persuade — in line with NexWell's clinical ethics standard
- • JCI-accredited partner clinics with specialist implantologists